Summary of Estimated Costs
The cost of fistula surgery in Karachi depends on the type and complexity of the case. Laser surgery is more advanced and costs higher, while open surgery is less expensive but requires longer recovery.
| Condition | Anal Fistula (Bhagandar — بھگندر) |
| Specialist | Dr. Abdullah Iqbal — MBBS, FCPS, Laser Proctologist, Karachi |
| Techniques Available | FiLaC, LIFT, VAAFT, Fistulotomy, Fistulectomy, PILTEC, Fistula Plug |
| Laser Surgery Cost | PKR 130,000 – 250,000 (depending on complexity) |
| Open Surgery Cost | PKR 70,000 – 80,000 |
| Recovery (Laser) | 3–5 days to routine | Full healing 4–8 weeks |
| Recovery (Open) | 4–6 weeks with wound dressings |
| Location | Hill Park General Hospital & MediCenter, Karachi |
| Last Reviewed | March 2026 by Dr. Abdullah Iqbal |
Anal fistula (bhagandar) is a chronic anorectal condition that requires surgical treatment — it does not resolve on its own. Dr. Abdullah Iqbal is a laser proctologist in Karachi with over 16 years of experience, holding MBBS and FCPS qualifications, and has performed more than 10,000 anorectal procedures including complex fistula surgeries using FiLaC, LIFT, VAAFT, and PILTEC techniques.
Every week I meet patients who have been silently suffering from a fistula for months or even years — delaying treatment out of embarrassment or hoping it will heal on its own. I want to be clear: with the right diagnosis and the right technique, anal fistula is very treatable, and laser surgery today means most patients go home the same day with minimal pain and a fast recovery. If you are looking for fistula treatment in Karachi, you are in the right place.
I trained in general surgery, then specialised in colorectal surgery and laser proctology. I have treated thousands of fistula cases — from simple intersphincteric tracts to high complex horseshoe fistulas that had recurred after previous surgery elsewhere. My team and I at Karachi Piles Clinic, Hill Park General Hospital are here to help you get a permanent solution.
A fistula is an abnormal tunnel that forms under the skin, connecting the inside of the anal canal or rectum to an opening on the skin near the anus. Most people develop it after an anal abscess (a pocket of infection and pus). Approximately 50% of perianal abscesses go on to form a fistula tract if not fully treated.
Sometimes a fistula develops gradually without a clear abscess episode. The hallmark sign is a small opening near the anus that persistently drains pus, blood, or foul-smelling fluid. A fistula tract has a lined wall that the body cannot close on its own — the tract must be surgically cleared or sealed for permanent healing.
Fistulas are classified based on their relationship to the anal sphincter muscles — the muscles that control bowel continence. This classification is critical because it directly determines which surgical technique is safest for your specific case. I map every fistula using MRI before planning treatment.
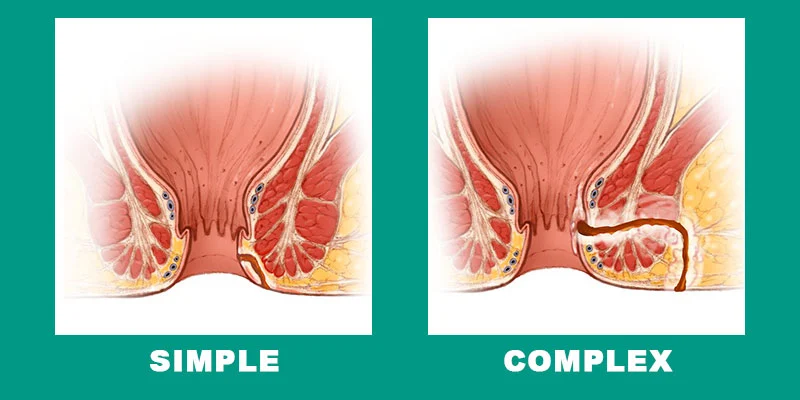
Another important classification divides fistulas into simple and complex based on tract size, number of openings, sphincter involvement, and treatment history. This distinction directly determines whether a one-stage or two-stage surgical approach is needed.
Simple Fistula: A low-lying tract that crosses little or no sphincter muscle — typically less than one-third of the external sphincter. All intersphincteric fistulas and low transsphincteric fistulas involving less than 30% of the external sphincter are classified as simple. These are suitable for single-stage laser treatment with excellent outcomes.
Complex Fistula: A high, multi-branched, or recurrent fistula that involves significant sphincter muscle and carries a risk of incontinence if treated aggressively in one sitting. A fistula is classified as complex if it meets any of the following criteria:
I always determine simple versus complex classification at your first visit so I can explain clearly which treatment pathway is safest for you.
If you are reading this, you may already be experiencing one or more of the following. These are the most common symptoms that bring patients to my clinic for fistula assessment:
If these symptoms recur, do not delay. Early treatment of a fistula is almost always simpler, less expensive, and more successful than treating a fistula that has been left to enlarge or develop branches. Book an appointment for an assessment.
Understanding the cause of your fistula is important — it helps treat any underlying condition and reduces the risk of recurrence after surgery.
Blocked Anal Glands (Most Common): Small glands inside the anal canal can become blocked and infected, forming an abscess that eventually burrows through tissue to create a fistula tract.
Unresolved Perianal Abscess: If a perianal abscess is not properly drained — or if it was drained but the underlying gland was not addressed — a fistula tract typically forms as the body creates a persistent drainage channel. Around half of all perianal abscesses lead to fistula formation.
During your consultation, I take a thorough history specifically looking for bowel symptoms, weight loss, night sweats, or prior illness that may point to an underlying cause that needs to be treated alongside the fistula.
Accurate diagnosis and complete mapping of the fistula tract is the most critical step — it is what determines which technique will give you the best outcome with the least risk.
I examine you gently in a private setting using a gloved finger to assess the external opening, check for discharge, and feel for the subcutaneous cord. I then use a small anoscope to inspect the internal opening inside the anal canal.
For complex or branching tracts, I order an MRI fistulogram — the gold standard imaging investigation that provides a precise three-dimensional map of the tract’s length, depth, and relationship to the sphincter muscles. For patients where I suspect underlying inflammatory bowel disease, I may also order a colonoscopy or blood tests including TB workup.
Thorough pre-operative mapping is what separates a successful fistula surgery from one that recurs. I never operate on a fistula without knowing exactly what I am dealing with.
Fistula does not heal without surgery. The fundamental goal of all fistula surgery is to eliminate the infected tract while protecting the anal sphincter muscles and preserving bowel continence. The method I recommend depends on the type and complexity of your fistula, your overall health, and your history of any previous fistula treatment.
At my clinic I use both standard open techniques and laser-assisted fistula surgery. For the large majority of patients, a laser-based approach offers less post-operative pain, faster return to normal activities, and no need for wound dressings.
I open the entire fistula tract along its length, allowing it to heal flat from the base as a scar. Fistulotomy is the simplest technique with the highest success rate for low, simple fistulas involving minimal sphincter muscle. It is not appropriate when significant muscle is at risk.
I excise the entire fistula tract and use laser energy to seal the edges, reducing bleeding and accelerating healing. This is suitable for simple fistulas where complete removal of the infected tract is desired.
LIFT is an excellent sphincter-sparing technique for transsphincteric fistulas. I access the intersphincteric plane, ligate (tie off) the internal opening, and curettage the outer portion — without cutting any sphincter muscle. I also perform Laser-assisted LIFT (LIFT + FiLaC) for superior closure rates.
A precision radial-emitting laser fiber is passed through the external opening and advanced along the entire fistula tract. The laser energy destroys the tract lining from within and seals it shut. There is no external cut, no wound to dress, and patients typically return home the same day. FiLaC success rates exceed 90% for simple fistulas in experienced hands.
I insert a thin fistuloscope to directly visualise the inside of the tract, cauterise it under vision, and close the internal opening with sutures. The outer skin remains intact. VAAFT has a recurrence rate of approximately 30% but remains a valuable option for selected complex cases where preserving tissue is the priority.
A bio-absorbable plug made from porcine or synthetic material is inserted into the fistula tract. The body gradually grows tissue around it. The procedure is nearly painless with minimal recovery, but plug displacement or infection remains a limitation in some cases.
A technique I use for very complex, multi-branched, or recurrent fistulas. PILTEC is an advanced evolution of LIFT combined with laser steps that I studied under international experts. I have achieved consistent results with this technique even in cases that had failed previous surgeries elsewhere.
Whether your fistula is treated in one sitting or two depends entirely on its complexity.
One-Stage Procedure: Ideal for simple, low fistulas with a single straight tract. The entire fistula is treated in a single operation — typically with FiLaC (Fistula Laser Closure) or laser-assisted fistulectomy. Healing is faster and post-operative discomfort is minimal.
Two-Stage Procedure (For Complex Fistulas): If your fistula is high, has multiple branches, or involves significant sphincter muscle, a two-stage approach protects continence and improves long-term results:
Laser fistula surgery with Dr. Abdullah Iqbal ranges from PKR 130,000 to PKR 250,000. The final amount depends on the following factors:
Open conventional fistula surgery in Karachi costs approximately PKR 70,000 to 80,000. However, open surgery involves longer hospital stay, painful wound dressings for 4 to 6 weeks, and a significantly longer recovery period.
Summary of Estimated Costs
The cost of fistula surgery in Karachi depends on the type and complexity of the case. Laser surgery is more advanced and costs higher, while open surgery is less expensive but requires longer recovery.
Fistula recurrence most commonly occurs when a branch of the tract was missed during surgery, when underlying infection was not fully resolved, when an underlying cause such as Crohn’s disease or tuberculosis was not identified and treated, or when post-operative care was inadequate. This is why I always perform MRI mapping before surgery and follow every patient personally until complete healing is confirmed.
Most patients return to routine within 3 to 5 days of laser surgery. Full internal healing takes 4 to 8 weeks. I see every patient personally at their follow-up visits until healing is complete. For a detailed guide on what to expect, read our expert advice on fistula surgery and recovery.
Choosing the right surgeon for fistula treatment matters enormously — an incomplete or poorly planned operation is the most common reason fistulas recur. Here is what makes my approach different:
An untreated anal fistula is not merely a small inconvenience — it is an active, ongoing infection that can spread, form new branches, develop into a complex horseshoe fistula, or cause a large perianal abscess requiring emergency surgery. Some patients have been draining pus for years, and by the time they reach me the tract has become significantly more complex than it was at the start.
I understand the embarrassment around these conditions. I deal with this every day and my clinic maintains complete patient privacy at all times. Every patient is treated with respect and dignity. Please do not wait until your fistula becomes a surgical emergency. Book a consultation — an early, simple fistula is almost always treatable in a single laser session.
Laser fistula surgery in Karachi costs between PKR 130,000 and PKR 250,000. Simple single-stage fistulas typically cost PKR 130,000 to 180,000. Complex or two-stage fistulas requiring seton placement followed by FiLaC laser closure range from PKR 200,000 to 250,000 or more. The laser fiber itself accounts for approximately 60% of the surgical cost as it is a single-use imported device. Open conventional fistula surgery costs PKR 70,000 to 80,000 but requires significantly longer recovery with wound dressings for 4 to 6 weeks.
After laser fistula surgery, most patients return to normal daily activities within 3 to 5 days. Complete internal healing typically takes 4 to 8 weeks depending on fistula complexity. Open conventional surgery requires 4 to 6 weeks before returning to normal activities, with wound dressings needed throughout that period. Laser procedures eliminate the need for dressings and significantly reduce post-operative pain compared to traditional surgery.
Office workers and desk-job employees typically need 3 to 7 days off after laser fistula surgery. Patients with physically demanding jobs — labourers, those who stand for long hours, or those who drive long distances — may need 2 to 3 weeks. Most laser fistula procedures are performed as day-care operations, meaning patients are discharged the same day without hospital admission.
Not all anal fistulas can be prevented, but risk can be reduced significantly. The most effective prevention is prompt and proper treatment of perianal abscesses before they form a fistula tract. Managing underlying conditions such as Crohn’s disease, tuberculosis, or inflammatory bowel disease also lowers fistula risk. Maintaining a high-fibre diet, good anal hygiene, and adequate hydration supports overall anorectal health.
No. Anal fistulas do not heal without surgical intervention. The fistula tract has a lined epithelial wall that the body cannot close spontaneously. Antibiotics may temporarily reduce associated infection or discharge but will not close the tract. Creams, home remedies, and herbal treatments provide no cure. For a detailed look at what does and does not work, read our article on healing a fistula without surgery. Surgical intervention — whether fistulotomy, laser FiLaC, LIFT, or VAAFT — is the only definitive treatment for anal fistula.
Success rates depend on procedure type and fistula complexity. For simple fistulas treated with FiLaC laser closure, success rates exceed 90 to 95%. For complex fistulas managed with a two-stage LIFT plus laser approach, rates remain between 85 and 95% in experienced hands. VAAFT has a recurrence rate of approximately 30% but remains suitable for selected complex cases. In my practice, recurrence rates for laser procedures are consistently below 5%.
With complete pre-operative MRI mapping and meticulous surgical technique, recurrence rates are less than 5% for simple fistulas and less than 10 to 15% for complex multi-branched cases. The most common causes of recurrence are a missed branch of the tract, an untreated underlying condition such as Crohn’s disease or tuberculosis, or inadequate post-operative care. I perform MRI fistulogram on all complex cases before surgery specifically to minimise this risk.